Corticobasal degeneration is a disease that is classified as one of the so-called tauopathies. According to abbreviationfinder, the disease is sometimes referred to by the abbreviation CBD. In the context of corticobasal degeneration, components of the tau protein are deposited in the human brain. As a result, the ability of the brain to function becomes increasingly impaired over time. Basically, corticobasal degeneration is a so-called atypical Parkinson’s syndrome.
What is corticobasal degeneration?
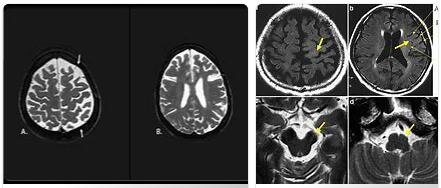
Imaging procedures show atrophies in the area of the cerebral cortex. So-called ballooned nerve cells also occur. The accumulations of the tau proteins can be determined with appropriate tissue examinations.
In principle, the typical symptoms can easily lead to confusion between corticobasal degeneration and Parkinson’s disease. In fact, corticobasal degeneration is a form of atypical Parkinson’s disease. These diseases are often confused with Parkinson’s.
In addition, corticobasal degeneration ranks third in terms of the frequency of atypical Parkinson’s syndromes, after multiple system atrophy and progressive supranuclear paresis. Corticobasal degeneration usually develops over a long period of time.
It leads to continuously increasing damage to the brain and its function. For this reason, corticobasal degeneration is a so-called neurodegenerative disease. The tau protein accumulates in the brain, which is also known as tauopathy in medical terms.
The central symptoms are similar to or correspond to the symptoms of Parkinson’s disease. In addition, the cognitive abilities of the affected persons progressively deteriorate. Basically, corticobasal degeneration is a relatively rare disease. According to current knowledge, the frequency is 1:100,000.
With regard to the characteristic symptoms, there are strong similarities to Parkinson’s. However, some symptoms of corticobasal degeneration also indicate a dementia disorder. However, the causes of corticobasal degeneration are different than in Parkinson’s disease, which is why it is counted among the atypical Parkinson’s syndromes.
Causes
Basically, corticobasal degeneration is a relatively rare disease. According to medical research results, the cause of the development of the disease lies in a special gene that is responsible for coding the so-called tau protein. The name of this gene is MAPT.
In the context of corticobasal degeneration, the tau protein accumulates in the brain of the affected person. The protein is primarily deposited in the area of the so-called frontal lobe. As the disease progresses, this deposit in the brain causes symptoms that are particularly associated with the death of so-called glial cells and neurons.
Symptoms, Ailments & Signs
Corticobasal degeneration is associated with certain symptoms and complaints in the affected patient. For example, an apraxia occurs, which is primarily related to the cerebral cortex. The cognitive performance of those affected also decreases over time.
Ultimately, those affected suffer from what is known as subcortical dementia. Corticobasal degeneration leads to an increase in muscle reflexes, and myoclonus is also possible. One of the typical symptoms of the disease is that the patients perceive their limbs as foreign and not part of the body. The English term for this phenomenon is ‘alien limb’.
In addition, there are various motor disorders that also occur in Parkinson’s disease. These complaints are often only one-sided at the beginning, for example hypokinesis or rigidity. In a few cases, a so-called resting tremor also occurs. In addition, dystonias are possible in the context of corticobasal degeneration, which primarily affect the neck or the limbs.
Some patients suffer from significant gait disturbance. In addition, some individuals exhibit facultative complaints. These include, for example, movement disorders of the eyes. Especially when dementia develops, anxiety and depression occur.
Diagnosis & course of disease
The diagnosis of corticobasal degeneration is based on a defined procedure. If a person shows symptoms typical of the disease, a doctor’s consultation is indicated. The doctor discusses the existing complaints with the patient. In the course of clinical examinations, the suspicion of corticobasal degeneration becomes more and more substantiated until finally a reliable diagnosis is made.
For example, histological laboratory tests of the brain are necessary. Imaging procedures show atrophies in the area of the cerebral cortex. So-called ballooned nerve cells also occur. The accumulations of the tau proteins can be determined with appropriate tissue examinations.
Complications
Corticobasal degeneration is one of the rare diseases that impair the functionality of the brain very quickly and severely. The reason for this is an increase in the components of the tau protein in the brain. This protein is preferentially deposited in the area of the frontal lobe.
As a result of the deposits in the brain, various neurons and cells in the central nervous system degenerate in affected patients. The course is similar to that of Parkinson’s disease. The complications arising from the neurodegenerative symptoms are serious. All cognitive abilities of the affected person deteriorate as the symptom progresses. There is a general disturbance of motor functions, especially walking, movement disorders of the eyes and speech difficulties.
This is followed by a rapid increase in muscle reflexes and muscle twitching. In a short time, signs of subcortical dementia become noticeable. Due to the severe physical and mental degeneration, those affected react with depression and anxiety. In addition, the patient is overcome by the feeling of regarding their own limbs as alien.
Corticobasal degeneration can only be detected by clinical procedures as well as imaging methods. There is currently no treatment for the symptom. It is limited to alleviating the suffering of those affected and maintaining their cognitive and mental abilities as far as possible. However, sick patients usually succumb to the symptom within a few years.
When should you go to the doctor?
If cramps and numbness are noticed in the muscles, corticobal degeneration may be the underlying cause. An appointment with the family doctor is indicated if the signs of illness increase and/or persist over a longer period of time. Should the characteristic feeling of strangeness appear in the muscles, medical advice is required. Signs of rigidity or hypokinesia also require rapid clarification by the general practitioner. Individuals who have been diagnosed with corticobal degeneration should see a doctor regularly. The individual symptoms must be treated by different specialists.
Depending on the symptom complex, these can be, for example, neurologists, orthopedists and physiotherapists. Due to the severity of the disease and the negative prognosis to be expected, a psychologist should also be consulted. Even if the course is positive, regular visits to the doctor are necessary, as new symptoms can develop again and again. In addition, the functioning of the brain tends to decline, which is why a neurologist must regularly carry out appropriate brain examinations. Externally, a corticobal degeneration is initially not recognizable. As the genetic disease progresses, poor posture and motor disorders can occur, which must be clarified by a doctor.
Treatment & Therapy
So far there are no therapeutic measures that are able to stop the progression of corticobasal degeneration. Typically, most patients die about one to eight years after the diagnosis of the disease. Possibilities for a cure are not yet known.
In some cases, the drug levodopa improves symptoms similar to Parkinson’s. Basically, the corticobasal degeneration proceeds in such a way that the affected patients suffer from increasing mobility disorders. Akinesia also occurs. Many people suffering from corticobasal degeneration ultimately die from inflammation of the lungs caused by lack of exercise.
Outlook & Forecast
The prognosis for the slowly but inexorably progressing corticobasal degeneration is poor. The symptoms of corticobasal degeneration are similar to those of Parkinson’s disease. However, as they progress, they are perceived as atypical Parkinson’s symptoms. The cognitive abilities of those affected are also increasingly declining. Their movements become increasingly slow.
Corticobasal degeneration is caused genetically. It occurs very rarely. Doctors treat it as an atypical parkinsonian syndrome. So far, however, there are no effective and independent therapeutic approaches to alleviate the symptoms of the rarely occurring corticobasal degeneration. The disease progresses without being slowed down or stopped with medication.
A characteristic feature for distinguishing corticobasal degeneration from Parkinson’s disease is that those affected perceive their own extremities as not belonging to them. The increasing dementia and the variety of symptoms occurring worsen the prognosis increasingly.
There is no treatment option for corticobasal degeneration. At best, the symptoms of Parkinson’s disease can be improved somewhat in some of those affected by drug therapies. However, the preparations administered often have a poor effect in this atypical Parkinson’s disease.
The increasing movement disorders occurring are making patients less and less mobile. As a result of increasing sedation, many sufferers die of pneumonia within a period of between one and ten years after diagnosis.
Prevention
According to the current state of medical knowledge, corticobasal degeneration cannot be prevented. Because the development of the disease is related to a genetic component over which the affected persons have no influence.
Aftercare
In most cases, patients with this disease have only a few follow-up measures available. First and foremost, the disease should be diagnosed quickly and at an early stage in order to prevent further complications or symptoms. As a rule, self-healing is not possible, so that the person affected should always consult a doctor if the symptoms of the disease appear.
The earlier the disease is detected, the better the further course is in most cases. In most cases, patients are dependent on taking various medications. The instructions of the doctor must always be observed, whereby the correct dosage and regular intake must also be observed.
If anything is unclear, you have questions or if you have any side effects, you should always consult a doctor first. Furthermore, those affected should protect their lungs particularly well, as this disease can often lead to inflammation. In most cases, the life expectancy of those affected is severely limited due to the disease. It is not uncommon for loving and empathetic conversations with one’s own family to be very important in order to prevent depression and other psychological problems.
You can do that yourself
Self-care options are relatively limited in individuals with corticobasal degeneration. Those affected suffer from an enormous impairment of their quality of life and are no longer able to cope with their everyday life independently. In particular, the rapid decline in cognitive performance and the disturbances in the motor area mean that patients with corticobasal degeneration are dependent on the help of other people for care and nursing.
Due to the difficulty in walking, patients are usually forced to use a wheelchair. In order to improve the quality of life, people are adapting and redesigning their homes for wheelchair use. As a result, those affected still retain some of their independence. In addition, the patients perform physiotherapy with a physiotherapist, thereby improving their motor skills and fitness. Sporting activities usually have a positive effect on the mental and emotional state. However, these must be coordinated with a doctor and are also not able to completely stop the progression of corticobasal degeneration.
To this day, corticobasal degeneration cannot be cured, so some patients suffer from anxiety attacks and depression, which are also caused by the serious physical changes.