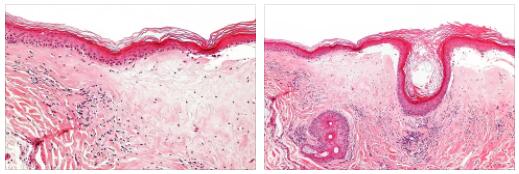
LS stands for lichen sclerosus which is a rare skin disease with inflammation-related changes in the connective tissue, the cause of which is assumed to be a dysregulation of the immune system. Lichen sclerosus affects women 5 to 10 times more often than men.
What is lichen sclerosus?
In the affected adolescents and adults, lichen sclerosus usually manifests itself through intermittent itching or burning and stinging in the genital area. See AbbreviationFinder for abbreviations related to Lichen Sclerosus.
Lichen sclerosus is a rare chronic inflammatory connective tissue disease that is probably due to a dysregulation of the immune system (autoimmune disease).
Lichen sclerosus usually manifests itself in the genital area, more rarely in extra-genital areas such as the hands, arms or back (about 10-15%). While in women the labia (labia), clitoris, clitoral hood and the perianal area (region around the anus) are primarily affected, lichen sclerosus in men manifests itself on the foreskin (prepuce), glans (glans penis) and only occasionally in the perianal area.
Lichen sclerosus is characterized by a porcelain-like, white discoloration of the skin with reactive thickening of the epidermis (keratinization), which is caused by sclerosing (inflammation-related proliferation) of the underlying connective tissue.
As a result of the sclerotic atrophy (tissue thinning) of the affected skin areas, phimosis (narrowing of the foreskin) can develop in men and shrinkage of the labia or clitoris in women, which leads to pain during sexual intercourse. Pruritus (itching), urethral strictures with painful urination and vaginal stenosis are other possible symptoms of lichen sclerosus.
Causes
The etiology of lichen sclerosus is still largely unknown. A multifactorial genesis of the disease is assumed in the presence of a genetic predisposition, although no familial accumulations can be observed.
In all likelihood, lichen sclerosus is due to a dysregulation of the immune system (autoimmune disease). In the course of several studies, reactivity against ECM1, an extracellular matrix protein, could be detected in the serum of the majority of those affected. The factors that trigger these dysregulated processes are still unknown. Trauma (including sexual abuse, scratching) are considered possible trigger factors.
In addition, lichen sclerosus is associated in almost 30 percent of cases with other autoimmune diseases such as Hashimoto’s thyroiditis, type 1 diabetes mellitus, asthma, lupus erythematosus, autoimmune gastritis, circular hair loss (alopecia areata) and vitiligo (white spot disease). Borrelia (bacteria that cause Lyme disease) are also being discussed as triggers for lichen sclerosus.
Symptoms, Ailments & Signs
In the affected adolescents and adults, lichen sclerosus usually manifests itself through intermittent itching or burning and stinging in the genital area. In addition, skin changes can occur that are initially reminiscent of a fungal infection. Problems during sexual intercourse, especially penetration, are also characteristic.
Some women experience severe soreness in their intimate area after intercourse. This can last for a few days and can be associated with bladder problems, pain and inflammation. In men, white, slimy deposits that smell unpleasant form in the penis area.
Painful skin lesions can form, which first appear on the foreskin and then spread to the glans and the entire penis. In children, lichen sclerosus becomes noticeable through a symmetrical reddening of the genitals. The symptoms of the disease usually appear suddenly and increase in intensity as the disease progresses.
Eventually, severe pain and noticeable skin changes appear. If lichen sclerosus is treated early, the symptoms usually subside after a few days or weeks. If not treated adequately, ulcers and scars may develop in the affected area.
Diagnosis & History
An initial suspicion of lichen sclerosus usually results from the characteristic symptoms (above all the porcelain-like, white scarring of the skin) and a gynecological examination with the colposcope (microscope to check the vagina and cervix).
The diagnosis is backed up by a biopsy (taking a sample from the affected skin area with a punch cylinder) with subsequent histological (histological) analysis. The histological findings also serve to rule out malignant degeneration and to differentiate lichen sclerosus from partially comparable diseases such as genital mycosis or localized scleroderma (including morphea).
Lichen sclerosus is classified as a chronic disease that cannot be cured and progresses in phases, with symptom-free intervals between the phases. If left untreated, lichen sclerosus leads to atrophy, chronic itching and synechiae (adhesion of tissue layers) to degeneration of the affected skin areas.
Complications
This disease causes patients to suffer from various ailments, all of which are very uncomfortable and can lead to a reduced quality of life. Those affected suffer from itching and itchy sores. Wound healing is also delayed by this disease, so that infections or inflammation can occur more often.
It is also not uncommon for pain to occur when urinating. These are burning and often lead to psychological problems or depression. It is also not uncommon for bleeding to occur on the skin. In men, the disease can also cause problems in the genitals and especially in the foreskin. This can also lead to restrictions in sexual intercourse.
Treatment of this disease is usually carried out with the help of medication. Complications usually do not occur and the disease progresses positively. However, treatment does not reduce recurrence of this disease. The life expectancy of the affected person is not reduced. Likewise, the affected person has to do without various care products in order to stabilize the skin in the affected areas.
When should you go to the doctor?
In most cases, abnormalities in the genital area are indications of an existing disease. A doctor’s visit is advisable if existing symptoms persist unabated for several days or weeks. If the symptoms increase in intensity or spread further, a doctor’s visit is required immediately. If there is pain or a burning sensation on the skin, a doctor is needed. If itching or open wounds occur, a doctor’s consultation is necessary. Pathogens and germs can get into the organism through the open wounds and trigger further diseases.
In severe cases, there is a risk of blood poisoning and thus a life-threatening condition. A doctor’s visit is therefore advisable in the event of pus formation, fever or general malaise. If a feeling of soreness develops after intercourse, this should be observed. In the case of slimy deposits or an unpleasant body odor in the intimate area, a doctor’s visit is required. Reddening of the skin, swelling or bleeding should be examined and treated. If women have irregular menstrual cycles, they should consult a doctor. If sexual dysfunction occurs in men or women, a doctor should be consulted. Likewise, when a man notices changes in the foreskin. If ulcers or scars develop, the observations should be discussed with a doctor.
Treatment & Therapy
In the case of lichen sclerosus, the therapeutic measures are primarily aimed at alleviating the symptoms. For this purpose, highly potent topically applied corticosteroids (including clobetasol propionate) are used as part of a shock therapy with high initial doses.
Another treatment option is treatment with calcineurin antagonists such as pimecrolimus or tacrolimus for immunosuppression. Although advanced atrophy cannot be reversed with the drugs mentioned, the progression of the disease is slowed down and, in the best case, stopped. While testosterone ‘s previously believed efficacy has not been proven, topical progesterone treatments for lichen sclerosus are being tested in clinical trials.
In addition, greasy creams (water-in-oil creams), ointments or oils are recommended for additional care of the affected skin areas and stabilization of the skin barrier while at the same time avoiding irritating shower lotions, soaps or perfumes. If there are also infectious diseases, they should be treated with appropriate anti-infective means (including antimycotics or antibiotics).
While the inflammatory processes in women can only be controlled and restricted and surgical measures such as vulvectomy or skin transplants are not used today due to the high recurrence rate, circumcision (circumcision) is used in most cases in men with lichen sclerosus and the presence of phimosis. which can often stop the disease.
Outlook & Forecast
Lichen sclerosus is a chronic disease, especially in girls and women, which in most cases cannot be cured. As a result, it is lifelong and only the typical symptoms of the disease can be alleviated with a well-adjusted therapy. The earlier treatment is started, the easier it is to control the disease. If lichen sclerosus is diagnosed late, the therapy proves to be more difficult, because in most cases complications such as internal adhesions have already occurred. To date, no cure is possible, especially in adult women. Curing by circumcision is conceivable for both boys and men.
Basically, lichen sclerosus is a benign disease. However, the risk of developing skin cancer is increased. For this reason alone, those affected should visit the dermatologist regularly in order to have malignant changes in the skin recognized and treated at an early stage.
The current therapy options do not have the same effect on all patients, which is why the general level of suffering is very individual from patient to patient. Careful care of the affected skin areas during and also outside of the flare-ups is very important for a favorable prognosis.
Prevention
Since the causes and trigger factors for lichen sclerosus have not yet been clarified, the disease cannot be prevented. However, certain forms of lichen sclerosus (including the hyperplastic variant) are considered non-infection-associated risk factors for malignant degeneration (squamous cell carcinoma), which is why those affected, especially women, should have regular medical examinations.
Aftercare
The aftercare measures for skin diseases usually depend very much on the exact disease, so that no general prediction can usually be made. The same applies to the disease lichen sclerosus: The earlier this disease is recognized and treated by a doctor, the better the further course, which is why the person concerned should consult a doctor as soon as the first symptoms and signs appear.
Follow-up care focuses on strengthening the weakened immune system and thereby accelerating the recovery process. Relaxation exercises can help, as can avoiding stress. A high standard of hygiene can have a positive effect on the course of such diseases. In most cases, treatment is by using creams or ointments and taking medication.
The person concerned should pay attention to regular use and the right dosage in order to permanently relieve the symptoms. Regular check-ups by a doctor are very important.
You can do that yourself
When treating lichen sclerorus, the focus is on alleviating the symptoms. In addition to various medications, conservative means from the household and nature as well as some self-help measures are used for this purpose.
The most important measure is to prevent seizures. This is achieved by identifying and avoiding any causes and triggers. A change in diet is particularly important. Patients should talk to a specialist about this and also consult other affected people. This makes it possible to quickly determine which individual triggers are present. Individuals suffering from lichen sclerosus should maintain a healthy lifestyle overall. Regular exercise, getting enough sleep, avoiding stress and other measures that strengthen the immune system can significantly reduce the symptoms of this rare skin disease.
Since certain forms of lichen sclerosus carry an increased risk of cancer, those affected should have regular medical examinations. It is advisable to consult a specialist at an early stage and work out a suitable therapy together with him. In addition, the measures mentioned must be carried out regularly in order to avoid an attack and the associated symptoms.